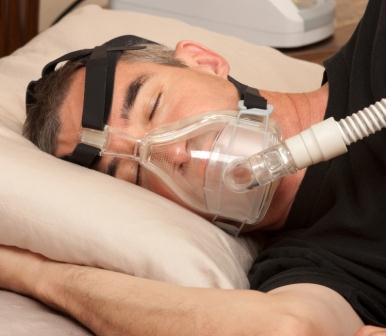
A trial of a simple yet effective surgery has led Australian experts to promote it as an option to specialists around the world for managing difficult obstructive sleep apnoea (OSA) cases.
After rigorous evaluation of the surgery, excellent outcomes were shown in sleep apnea patients who had been unable to use continuous positive pressure airway (CPAP) treatment, with patients achieved relief from snoring and disrupted sleep and experienced improved general health. according to a new report in the Journal of the American Medical Association (JAMA).
Up to 1 billion people are estimated to have OSA globally, with the main treatment CPAP tolerated by only half of those who try it. Almost 30% of people with OSA wake up very easily with light sleep and other problems caused by minor airway narrowing.
The multi-level surgical technique combining a new version of palate surgery with a low risk tongue procedure to create an improved airway resulted in a substantial reduction in the number of night-time apnea events and improvements in daytime sleepiness and quality of life. After removing any tonsils, the palate is repositioned and the tongue treated to open up the airway and reduce obstruction.
Flinders University’s Emeritus Professor Doug McEvoy says the surgery offers promise to millions of people around the world who suffer from obstructive sleep apnoea but cannot adapt to using a CPAP mask or similar device each night.

“This trial is the result of extensive prior research into the surgical treatment of sleep apnoea and gives new hope to people who, without treatment, would each day continue to feel sleepy and depressed and may have their lives cut short by the detrimental effects of long-term interrupted sleep,” says Professor McEvoy.
Lead author University of Wollongong Professor Stuart MacKay, who will give further details of the surgical clinical trial at the global online European Respiratory Society congress on 7 September and in a JAMA podcast, says about half of patients prescribed CPAP treatment are not using it consistently long term.

“It’s very exciting to see so many patients getting a better night’s sleep with reduced snoring and less health risk after this surgery,” says Professor MacKay.
The paper, ‘Effect of Multilevel Upper Airway Surgery vs Medical Management on the Apnea-Hypopnea Index and Patient-Reported Daytime Sleepiness Among Patients with Moderate or Severe Obstructive Sleep Apnea: The SAMS Randomized Clinical Trial’ (2020) by S MacKay, AS Carney, PG Catcheside, CL Chai-Coetzer, M Chia, PA Cistulli, J-C Hodge, A Jones, B Kaambwa, R Lewis, EH Ooi, AJ Pinczel, N McArdle, G Rees, B Singh, N Stow, EM Weaver, RJ Woodman, CM Woods and A Yeo, RD McEvoy, has been published in JAMA. DOI: 10.1001/jama.2020.14265
Key points
- The trial participants were recruited from six clinical centres in three Australian states (SA, NSW and WA) and were predominantly overweight males with severe OSA who could not satisfactorily use standard medical treatments.
- Of the 102 people in the trial, 51 were randomly assigned to receive the OSA surgery, the other 51 to continue with best possible medical treatment.
- After six months, those receiving the surgery had an approximate 60% decrease in the frequency of throat obstructions at night compared with a 20% decrease in participants who remained on medical treatment, and, had major added improvements in snoring, daytime sleepiness and general health status.
- A total of seven surgeons performed the multilevel surgery across the six clinical centres using techniques pioneered in Australia by the late Dr Sam Robinson and subsequently refined and standardised for the trial by Professor Stuart MacKay and Professor Simon Carney.
- The trial was the brainchild of the late Professor Nick Antic, a Flinders University and SA Health respiratory and sleep specialist, who led the study until his death in 2016.
The project has been funded by the Australian Government NHMRC, Flinders University and The Repat Foundation.

