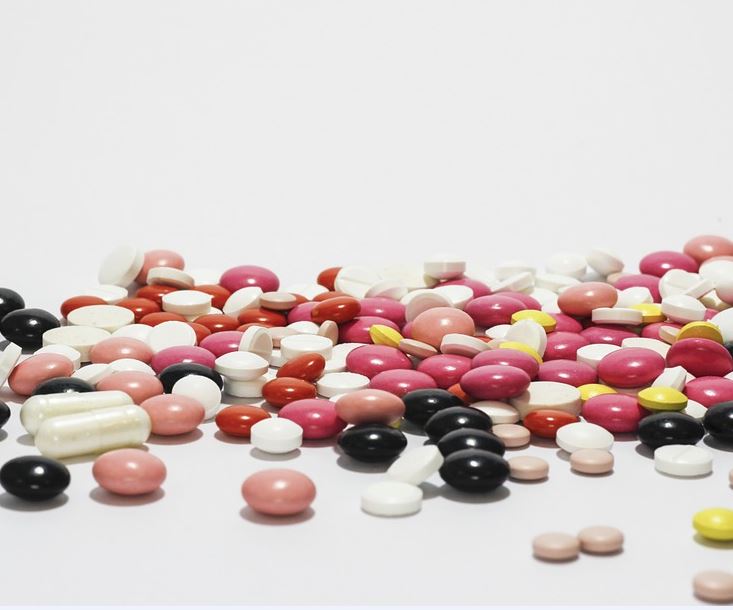
Along with over-the-counter opioid medicines, the use of prescription-only drugs such as oxycodone, fentanyl and morphine is on the rise.
From 1 February 2018, codeine-containing medicines will be rescheduled in Australia to curb rising rates of opioid dependency and accidental drug induced deaths through opioid use.
This will mean that the codeine-containing analgesic and cough medicines currently available over-the-counter will require a prescription.
Professor Ann Roche, Director of the National Centre for Education and Training on Addiction (NCETA) at Flinders University, says regular use of codeine can lead to addiction and serious health consequences.
“Codeine is an opioid drug closely related to morphine and, like morphine, is derived from opium poppies,” Professor Roche says.
“Codeine can cause opioid poisoning and in high doses, death. Regular use of medicines containing codeine, for example for persistent non-cancer pain, has led to some consumers becoming dependent on codeine without realising it,”
“The codeine-containing medicines that are currently available over-the-counter are usually combined with either paracetamol or ibuprofen. Long-term use of high doses of paracetamol can also result in liver damage.
“Adverse effects of long-term ibuprofen use include serious internal bleeding, kidney failure and heart attack. In addition, these medicines offer very little, if any, additional benefit when compared with medicines without codeine.”
Today NCETA is hosting a national seminar to focus on preventing and responding to harms associated with pharmaceutical opioid use in Australia.
Recent research has found that opioid use has more than doubled among Australians aged 35 to 44 since 2007, with the rate of associated accidental deaths on the rise.
More than two-thirds of these deaths were due to pharmaceutical opioids rather than heroin.
In addition, there are increasing concerns regarding problems such as pharmaceutical opioid dependence and inappropriate use for persistent non-cancer pain.
Professor Roche says there is also growing awareness of the potential side effects of long-term opioid use including hormone and sexual dysfunction, osteoporosis, depression and increased sensitivity to pain.
“Pharmaceutical opioids are very valuable medicines, however Australia is currently experiencing a range of harms associated with their use. We also need strategies to support codeine-dependent individuals who will no longer be able to obtain these medicines without a prescription,” says Professor Roche.
A further issue to be addressed, is the forthcoming introduction of online real-time monitoring of selected Schedule 8 (controlled) drugs, which will provide prescribers and pharmacists with a comprehensive overview of Schedule 8 opioid medicines a given patient is taking.
This is likely to identify a large number of individuals who have developed opioid dependence and other related problems and the seminar will identify approaches for addressing these issues.
The seminar aims to ensure that the state is appropriately prepared for future challenges in this area. It is funded by Indivior Pty Ltd, will bring together a range of experts and key stakeholders.
Speakers will include:
- Professor Ann Roche, Director NCETA
- Ms Maryann Elias, Senior Pharmacist, SA Drugs of Dependence Unit
- Dr Suzanne Nielsen, Pharmacist, Senior Lecturer, National Drug and Alcohol Research Centre, University of NSW
- Dr Tim Semple Deputy Head, Pain Management Unit, Royal Adelaide Hospital
- Dr Nico Clark, Clinical Director, Drug and Alcohol Services SA

